Scientists are tightening the case that a virus most people catch in childhood is not just associated with multiple sclerosis, but may actively set the disease in motion. A growing body of work now links the Epstein-Barr virus to immune cells that attack the brain and spinal cord, offering the clearest picture yet of how a common infection might trigger MS in a small subset of those it infects.
The emerging story is both unsettling and hopeful. It suggests that a nearly universal virus can help ignite a lifelong neurological illness, yet it also points to concrete targets for vaccines and therapies that could one day prevent MS before it starts.
The common virus under suspicion
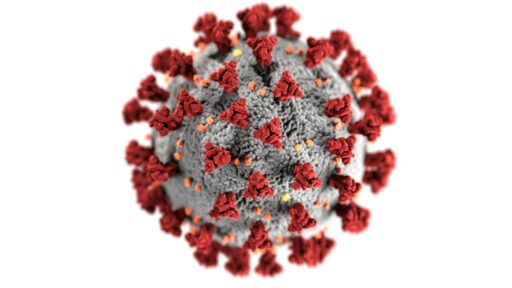
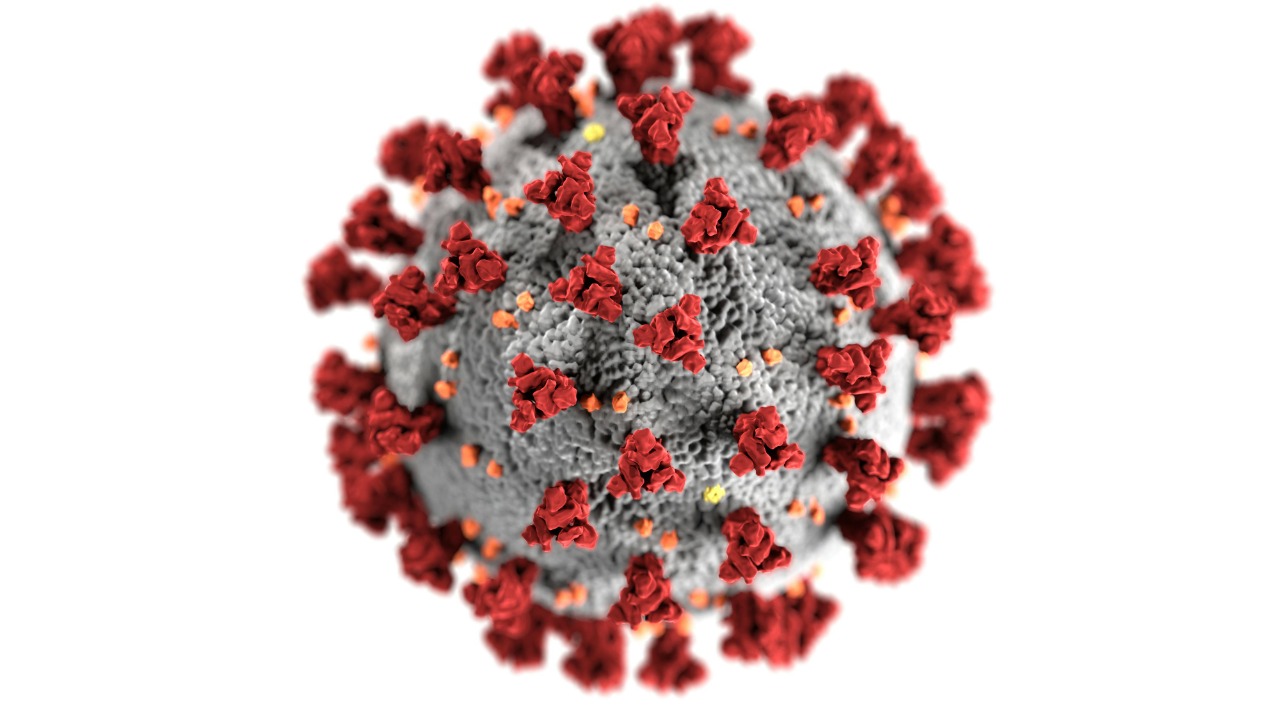
Epstein-Barr virus, often shortened to EBV, is so widespread that almost everyone encounters it early in life. In many people it causes no obvious illness, while others develop infectious mononucleosis, sometimes called mono, as described in analyses that connect Epstein Barr EBV to later neurological risk. For decades, researchers have suspected that this very common infection might have a darker side, because people with MS almost always show past exposure to Epstein-Barr virus while those without MS are less consistently infected.
Large epidemiological studies have now moved that suspicion closer to causation. One influential longitudinal Study design followed residual serum samples from 810 M patients with MS and matched controls, finding that Epstein-Barr infection preceded nearly every MS diagnosis and that new infection dramatically raised the odds of developing the disease. Additional work summarized in a report that states that Their findings in Science argue that Epstein-Barr virus may be a leading cause of multiple sclerosis, strengthening the case that EBV is not just a bystander but a key driver.
From association to mechanism: how EBV can trigger MS
Identifying a statistical link is one thing; explaining how a virus causes immune cells to attack myelin is another. Recent immunology studies are beginning to close that gap. Research highlighted by national health agencies reports that Infection with Epstein Barr virus dramatically increases the odds of developing multiple sclerosis, which prompted scientists to search for a biological explanation in the immune system itself.
Several teams have converged on the idea of molecular mimicry, in which antibodies or T cells raised against Epstein-Barr virus mistakenly target proteins in the brain. Work described in Science Advances found that some individuals produce antibodies against EBV that also recognize a protein in the central nervous system, a result summarized in coverage that notes that, according to the findings, According to the published in Science Advances Wednesday, these misdirected antibodies could help drive the balance and mobility problems associated with MS. Another set of experiments, led by William Robinson and colleagues, described how specific antibodies induced by Epstein-Barr virus can bind to nervous system proteins, as detailed in a Study identifies how EBV may prime the immune system to attack the nervous system.
The missing link inside the brain and spinal cord
The most striking new data focus on what is happening inside the central nervous system of people with MS. Investigators examining cerebrospinal fluid have identified expanded populations of CD8+ killer T cells that are sharply tuned to Epstein-Barr virus. In one recent analysis, scientists reported that, in MS patients, killer T cells that recognized EBV proteins were up to 100 times more abundant in the CSF around the brain and spinal cord, a dramatic enrichment described in a report that states that In MS these EBV specific cells dominate the local immune response.
Further work has characterized how these T cells behave. A study in Nature Immunology found that certain CD8+ killer T cells that respond to Epstein-Barr virus are more abundant in people with MS and may be particularly aggressive, as summarized in coverage of Nature Immunology findings. Complementary research on T cells in cerebrospinal fluid has shown that expanded lymphocytes in MS are specific for Epstein-Barr-virus-infected B cells, supporting mechanisms in which EBV infected cells in the brain act as targets that sustain inflammation, as described in work on Suggested mechanisms by which EBV might cause MS.
These cellular findings dovetail with new imaging and tissue studies. Scientists have reported that immune cells linked to Epstein-Barr virus cluster in MS lesions and appear to be activated locally, as described in a detailed analysis of immune cells linked to EBV that may play a role in MS. Another summary of recent work describes how Epstein-Barr virus may actively provoke the immune system in people with MS, with killer cells that normally destroy infected or damaged cells instead contributing to tissue injury, a pattern highlighted in a report on New research suggests that EBV can drive these destructive responses.
Genetic susceptibility and why only some people develop MS
One of the enduring puzzles is why almost everyone encounters Epstein-Barr virus, yet only a small fraction go on to develop MS. Genetic studies are beginning to fill in that gap. Researchers at the University of Zurich and collaborating centers have shown that Epstein-Barr virus together with a specific gene variant contributes to the onset of multiple sclerosis, indicating that infection alone is not enough and that certain inherited factors are required, as explained in a report where However certain gene variants also play an important role.
Broader reviews of MS risk factors now describe Epstein-Barr virus as a leading cause of multiple sclerosis, but emphasize that the virus acts in concert with genetic susceptibility and environmental exposures. One synthesis in a neurology journal notes that epidemiological data support EBV infection as a rare complication that can lead to MS, while other contributors such as vitamin D status and smoking still matter, as summarized in an Abstract Epidemiological overview. Patient focused organizations echo this complexity, explaining that while Epstein-Barr virus significantly increases the odds of developing MS, it does not cause MS on its own, a message reflected in guidance on Epstein Barr Virus EBV and MS.
What the EBV link means for prevention and treatment
The recognition that Epstein-Barr virus is deeply entwined with MS is already reshaping research priorities. Vaccine developers are testing whether blocking EBV infection in the first place could prevent MS decades later. One review describes how Moderna has launched the first trial of a human mRNA vaccine, mRNA-1189, that encodes five EBV envelope proteins (gp42, gp350, gB and others), with the early study beginning enrollment to assess safety and immune responses, as detailed in a report on the first trial by Moderna EBV vaccination.
Therapeutic strategies are also evolving as scientists connect specific immune pathways to Epstein-Barr virus. Clinicians already use disease modifying treatments to reduce relapses and slow progression in MS, and expert reviews describe how the latest drugs increasingly target underlying immune mechanisms rather than just symptoms, as summarized in an Expert opinion on disease modifying therapies. As research clarifies how EBV specific killer T cells and infected B cells interact in MS, future treatments may aim to selectively disarm those cells or clear latent Epstein-Barr virus from the body.
For patients and clinicians, the EBV story is changing how they think about risk. Educational materials now explain that infection with Epstein-Barr virus increases the risk of developing MS and that this virus may be a leading cause of the disease, as summarized in guidance that states that Complex Link What Epstein Barr EBV means for MS risk. At the same time, scientists caution that almost all Americans carry Epstein-Barr virus and only a minority will ever develop multiple sclerosis, a point echoed in summaries that describe how Multiple Americans live with EBV without neurological disease. The challenge now is to turn the new mechanistic insights into tools that can identify who is truly at risk and intervene before the first symptoms ever appear.